Diabetes affects the feet in ways that are often invisible until serious damage has occurred. Nerve damage (neuropathy) reduces sensation in the feet; consequently, a a blister, cut, or pressure sore may go unnoticed for days or weeks. Furthermore, poor circulation (peripheral artery disease) slows healing and increases the risk of infection. Together, therefore, these two processes create the conditions for diabetic foot ulcers — and ultimately, in unmanaged cases, amputation.
Consequently, the diabetic foot test — also called a diabetic foot screening or comprehensive foot examination — is one of the most important annual check-ups for every person living with diabetes. At MCR Diabetes & Eye Care, Kannur, our diabetologist performs thorough foot screenings as part of every comprehensive diabetes consultation. This guide explains each component of the test, what the results indicate, and what you can do at home between clinical screenings.
Why the Diabetic Foot Test Is Essential
Diabetic peripheral neuropathy — nerve damage caused by chronically elevated blood sugar — affects approximately 50% of people with long-standing diabetes. Notably, it often develops silently — specifically, a person may lose the ability to feel pain, pressure, or temperature changes in their feet without ever noticing. As a result, however, injuries that would normally cause immediate pain go undetected, worsen, and become infected.
The Chain of Events From Nerve Damage to Amputation
Understanding the sequence helps explain why early testing is so critical. First, prolonged high blood sugar damages the peripheral nerves in the feet and lower legs. Second, this nerve damage reduces protective sensation — the ability to feel pain that alerts you to injury. Third, without this warning system, minor injuries (a tight shoe rubbing, a small cut, a hot surface) cause damage that goes unnoticed. Fourth, poor circulation slows healing and allows infection to set in. Finally, uncontrolled infection can spread to bone (osteomyelitis) and may ultimately require amputation. Furthermore, research shows that 85% of diabetes-related amputations are preceded by a foot ulcer that was not identified and treated early enough.
Key fact: Both the International Diabetes Federation and the American Diabetes Association recommend a comprehensive foot examination at least once a year for every person with diabetes — more frequently for those with existing risk factors. However, fewer than 10% of people with diabetes in India currently receive regular foot examinations, according to clinical studies.
Who Is at Highest Risk for Diabetic Foot Problems?
While all people with diabetes are at some risk, several factors notably increase the likelihood of developing a serious foot problem. These include a diabetes duration of more than 10 years, poor long-term blood sugar control (HbA1c consistently above 8%), previous foot ulcers or amputations, current neuropathy symptoms such as numbness or tingling, peripheral artery disease, foot deformities such as claw toes or bunions, smoking or tobacco use, and wearing inappropriate footwear. Additionally, people who walk barefoot, work in manual labour, or have poor vision that makes foot self-inspection difficult are also at elevated risk.
What Tests Are Done During a Diabetic Foot Examination?
A comprehensive diabetic foot test is, in fact, not a single procedure — it is a structured examination comprising several complementary assessments. Each test evaluates a different aspect of foot health. Overall, they provide a complete picture of both nerve function and blood supply to the feet.
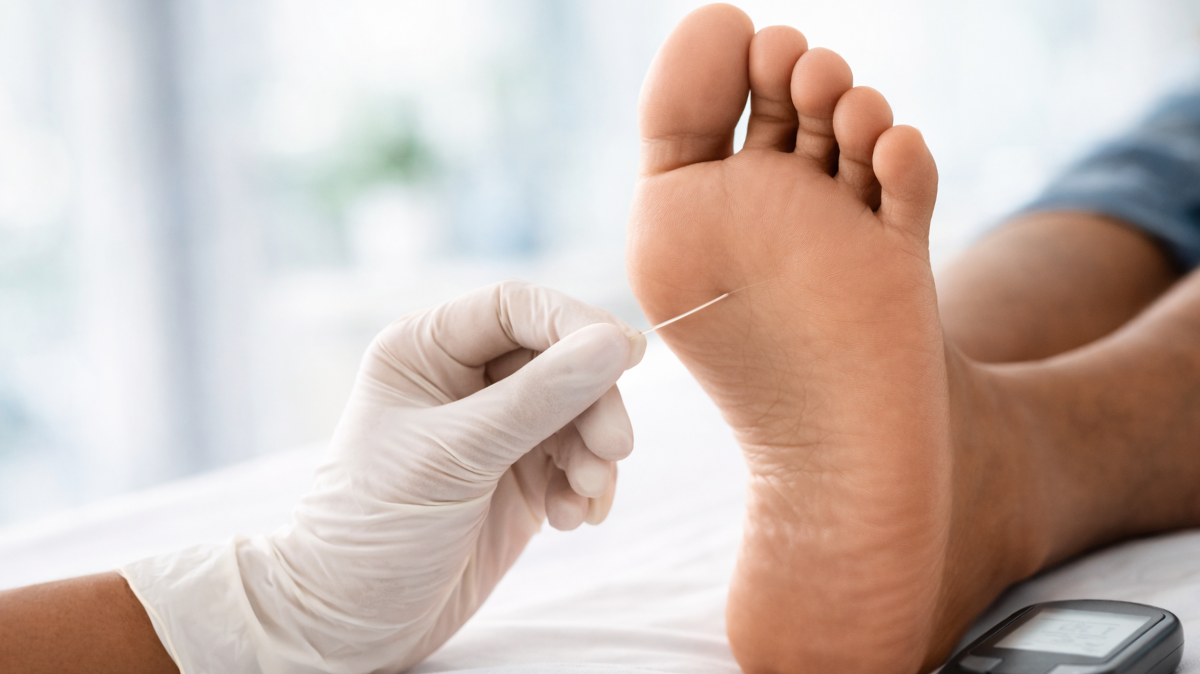
Test 1: The 10-Gram Monofilament Test
Monofilament Sensation Test
Neuropathy
Test 2: Vibration Perception Test (Tuning Fork or Biothesiometer)
Vibration Perception Test
Large-Fibre Neuropathy
Test 3: Ankle Reflexes (Neurological Assessment)
Ankle Reflex Test
Nerve Conduction
Test 4: Ankle-Brachial Index (ABI) — Circulation Assessment
Ankle-Brachial Index (ABI)
Circulation / PAD
Test 5: Visual Inspection and Dermatological Assessment
Visual and Dermatological Inspection
Skin & Structure
Test 6: Temperature Sensation Test
Furthermore, some specialised centres — including MCR Diabetes & Eye Care — also perform a temperature sensation test using a device called TipTherm, which has a warm end and a cool end. The inability, therefore, to distinguish between hot and cold on the feet is one of the earliest indicators of small-fibre neuropathy, often preceding the loss of touch sensation detected by monofilament. Identifying small-fibre neuropathy early is therefore particularly valuable because it provides a window of opportunity to prevent progression through improved blood sugar control.
Understanding Your Diabetic Foot Risk Classification
After completing all components of the foot examination, your diabetologist will subsequently, your diabetologist will assign a risk category based on the findings. This classification determines how frequently you need follow-up foot examinations and what preventive interventions are recommended.
IDF Diabetic Foot Risk Categories
| Category | Risk Level | Key Features | Recommended Review |
|---|---|---|---|
| Category 0 | Low Risk | Normal sensation, normal pulses, no deformity, no previous ulcer | Once a year |
| Category 1 | Moderate Risk | Peripheral neuropathy OR peripheral artery disease — but not both | Every 6 months |
| Category 2 | High Risk | Neuropathy AND peripheral artery disease; AND/OR foot deformity | Every 3 months |
| Category 3 | Very High Risk | Previous foot ulcer or amputation history — regardless of current findings | Every 1–3 months |
Important: Even Category 0 (low risk) does not mean no risk — it simply means risk is currently low with good sensation and circulation. Risk can change at any time, particularly if blood sugar control deteriorates. Therefore, annual re-screening is essential for everyone with diabetes, regardless of current risk category.
Warning Signs: When to Seek Immediate Medical Help
Between clinical foot examinations, it is therefore essential to recognise which symptoms require urgent medical attention rather than waiting for a scheduled appointment. In people with diabetes, furthermore, foot problems can deteriorate rapidly — what appears to be a minor wound can become a serious infection within days.
Symptoms That Require Prompt Medical Review
- Any open wound, sore, or ulcer on the foot
- Redness, warmth, or swelling around a wound
- Pus or discharge from any foot wound
- Black or darkened skin on the foot or toe
- Spreading redness or red streaks up the leg
- Fever accompanied by any foot problem
- A wound that has not improved in 2–3 days
- New numbness, tingling, or burning in feet
- Sudden loss of sensation in foot or toes
- Calluses or corns that are thickening rapidly
- Cracked heels that are deepening or painful
- Ingrown or infected toenails
- A blister — even if it appears minor
- Foot deformity that is worsening
Critical reminder: People with diabetic neuropathy may not feel pain even from serious foot injuries. Therefore, the absence of pain does not mean a wound is minor or safe to leave untreated. Any visible wound, however small, on the foot of a person with diabetes requires medical assessment — the same day if possible.
Daily Foot Self-Check: What to Do at Home Between Tests
Clinical foot testing is performed annually or more frequently depending on risk. However, equally important is the daily foot self-examination that every person with diabetes should perform at home. This simple habit, therefore, takes less than two minutes and can detect problems before they become serious.
The Daily 6-Step Foot Self-Check
Footwear and Foot Care: Preventing Problems Between Tests
Appropriate footwear is undoubtedly one of the most important — and most commonly neglected — aspects of diabetic foot protection. Indeed, the wrong footwear is implicated in the majority of diabetic foot ulcers, as pressure points and friction from ill-fitting shoes create wounds that neuropathy prevents the person from feeling.
Footwear Guidance for People with Diabetes
In particular, people with diabetes should wear well-fitted, closed-toe shoes with a wide toe box, cushioned insole, and no internal seams that could rub against the skin. Sandals and open-toed footwear leave the feet exposed to injury. Walking barefoot — even indoors — is dangerous for anyone with diabetic neuropathy. Furthermore, shoes should be purchased in the afternoon when feet are at their largest, and both feet should be measured, as they are often slightly different sizes. Specialised diabetic footwear and custom insoles are available for people with foot deformities or high plantar pressure.
Additional Foot Care Habits That Reduce Risk
In addition to footwear, several other daily habits significantly reduce the risk of diabetic foot complications. These include washing feet daily in warm (not hot) water and drying thoroughly — especially between the toes. Specifically, people with neuropathy should always test water temperature with the elbow, not the foot, as they may not detect scalding water. Additionally, never use sharp instruments to remove calluses or corns at home — always seek professional podiatric care. Keeping blood sugar well controlled remains the single most powerful strategy for slowing nerve and circulation damage in the long term.
Key point: Above all, excellent blood sugar control — maintaining HbA1c as close to your target as safely possible — is the most effective intervention for preventing diabetic neuropathy from worsening. For personalised guidance on achieving better blood sugar control, see our guide to blood sugar control tips or our comprehensive Indian diabetes diet chart.
Book Your Diabetic Foot Screening at MCR Kannur
When did you last have your feet examined by a diabetologist? If it has been more than a year — or if you have never had a foot screening — now is the time to act. Our specialist team at MCR Diabetes & Eye Care, Kannur, performs comprehensive diabetic foot tests as part of every diabetes consultation. Early detection protects your feet, your mobility, and your quality of life.
Frequently Asked Questions: Diabetic Foot Test
Below are answers to the most common questions about diabetic foot testing and foot care. If you have further questions, our team at MCR is always available to help.
What is a diabetic foot test?
What is the monofilament test for diabetic feet?
How Often and Why to Get Tested
The frequency of foot testing depends on your individual risk category. Annual testing is the minimum for all people with diabetes; however, those with neuropathy or circulation problems require more frequent review.
How often should a person with diabetes get a foot test?
More Questions About Diabetic Foot Health
The following questions address concerns about foot damage, warning signs, and what to expect during testing.
The following questions address additional concerns that many people with diabetes have about foot testing, foot damage, and foot care practices.
Can diabetic foot damage be reversed?
Recognising Warning Signs and Testing Experience
Knowing what to watch for between clinical appointments is as important as the tests themselves. The following questions address the warning signs of diabetic foot problems and what the testing experience involves.
What are the warning signs of diabetic foot problems?
Is diabetic foot testing painful?
Final Takeaway: Your Feet Deserve Annual Attention
Diabetic foot problems are, indeed, among the most serious yet most preventable complications of diabetes. Specifically, the diabetic foot test — taking just 10–15 minutes in a clinical setting — provides a comprehensive picture of nerve function, blood circulation, skin health, and structural integrity. Consequently, it can detect problems years before they become visible or painful, giving both patient and doctor the opportunity to intervene early and effectively.
Annual foot testing, combined with the daily self-check habit, is consequently and appropriate footwear, creates a powerful protective system around your feet. Furthermore, moreover, every improvement in blood sugar control — through better diet, regular exercise, medication adherence, and stress management — reduces the rate at which neuropathy progresses and therefore reduces the long-term risk of foot complications.
At MCR Diabetes & Eye Care, Kannur, comprehensive diabetic foot screening is an integral part of every diabetes review appointment. If you have not had your feet examined recently, we encourage you to act now — not later. For related guidance, explore our blogs on blood sugar control tips, home blood sugar testing, and the Indian diabetes diet chart — all of which contribute directly to protecting your foot health over the long term.